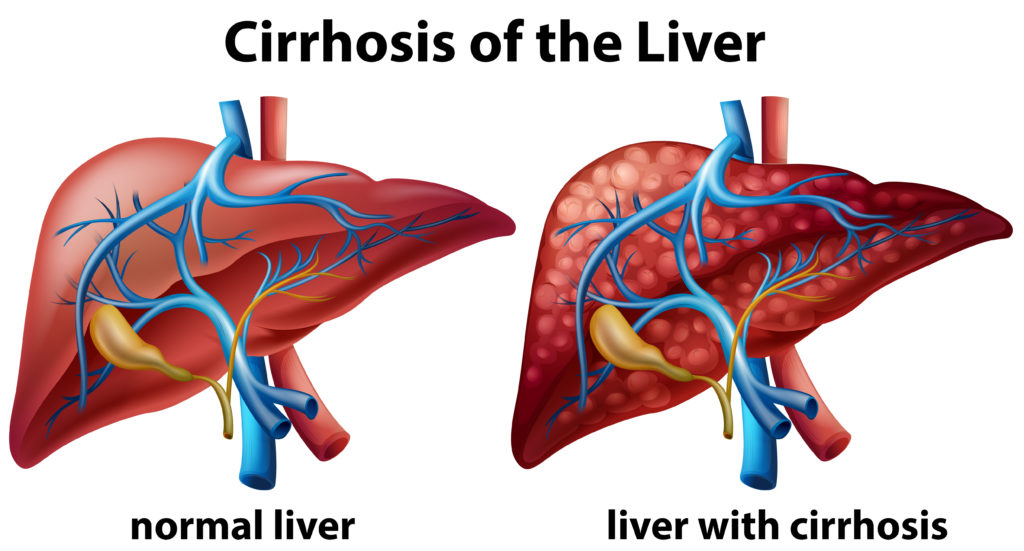
Liver Cirrhosis: Incidence, Symptoms, and Treatment
Liver cirrhosis is a late-stage liver disease characterized by scarring (fibrosis) of liver tissue, which disrupts the liver’s ability to function properly. The damage to the liver is progressive and often irreversible, leading to a significant decrease in its ability to process nutrients, hormones, drugs, and toxins, as well as produce proteins and other substances necessary for health. Cirrhosis is the result of long-term, continuous damage to the liver and may be due to many different causes, including chronic alcohol abuse, chronic viral hepatitis (hepatitis B and C), and fatty liver disease associated with obesity and diabetes.
Causes
Common causes of liver cirrhosis include:
- Chronic Alcohol Abuse: A leading cause of cirrhosis. The risk increases with the amount and duration of alcohol consumption.
- Chronic Viral Hepatitis: Particularly hepatitis B and C, which can lead to liver inflammation and, subsequently, cirrhosis.
- Non-Alcoholic Fatty Liver Disease (NAFLD): Associated with obesity, type 2 diabetes, and metabolic syndrome.
- Autoimmune Hepatitis: Where the immune system attacks liver cells, causing inflammation and scarring.
- Other Causes: Can include genetic diseases such as hemochromatosis (iron buildup in the body) and Wilson’s disease (copper accumulation in the liver), bile duct disorders, and certain medications.
Symptoms
In its early stages, cirrhosis often has no symptoms. As the disease progresses, symptoms may include:
- Fatigue and weakness
- Loss of appetite, weight loss
- Nausea, vomiting
- Abdominal pain and bloating (due to fluid accumulation)
- Jaundice (yellowing of the skin and eyes)
- Itching
- Swelling in the legs and ankles (edema)
- Easy bruising and bleeding
- Spider-like blood vessels on the skin
Complications
Cirrhosis can lead to several serious complications, including:
- Portal hypertension: Increased blood pressure in the portal vein, leading to varices (swollen blood vessels) that can bleed.
- Ascites: Accumulation of fluid in the abdomen.
- Hepatic encephalopathy: Impaired brain function due to the liver’s inability to remove toxins from the blood.
- Liver cancer: People with cirrhosis have an increased risk of developing liver cancer.
Diagnosis
Diagnosing cirrhosis involves a combination of medical history, physical examination, blood tests, imaging studies (such as ultrasound, CT scans, or MRI), and sometimes a liver biopsy to assess the extent of liver scarring.
Treatment
There is no cure for cirrhosis, but treatment can help manage symptoms and slow progression. Strategies include:
- Treating the underlying cause: Such as abstaining from alcohol, managing chronic viral hepatitis with antiviral medications, or controlling diabetes.
- Preventing complications: Monitoring and treating complications like portal hypertension, variceal bleeding, ascites, and hepatic encephalopathy.
- Lifestyle changes: Including a healthy diet, avoiding alcohol, and managing weight.
- Liver transplant: In advanced cases, a liver transplant may be considered when the liver function significantly deteriorates.
Prevention
Preventing liver cirrhosis largely involves minimizing risk factors:
- Avoid excessive alcohol consumption.
- Get vaccinated against hepatitis B and practice safe behaviors to reduce the risk of hepatitis C.
- Maintain a healthy weight and manage conditions like diabetes and high cholesterol.
- Avoid exposure to toxins and use medications responsibly.
Early detection and management of liver diseases can help prevent cirrhosis. If you have risk factors for liver disease, regular check-ups and liver health monitoring are crucial.
Why Choose London Private Ultrasound?
At London Private Ultrasound, we prioritize your health and comfort. Our team of experienced radiologists and healthcare professionals are dedicated to providing the highest quality of care. Here’s why you should choose us:
- Expert Radiologists: Our team consists of highly trained and experienced radiologists who are experts in ultrasound diagnostics.
- State-of-the-Art Technology: We use the latest ultrasound machines to ensure the highest level of accuracy in our scans.
- Patient-Centered Care: We focus on creating a comfortable and stress-free environment for our patients.
- Timely Results: We understand the importance of quick diagnosis and provide fast and reliable results.
- Convenient Location: Located in the heart of London, our clinic is easily accessible.
Book Your Ultrasound Scan Today
At London Private Ultrasound, we are committed to providing high-quality diagnostic services with a patient-centered approach. Our expert radiologists and cutting-edge technology ensure that you receive the best possible care.
Don’t wait to get the answers you need. Book your abdomen or pelvic ultrasound scan today by contacting us at:
Address: 27 Welbeck Street, London, W1G 8EN
Tel: 020 7101 3377
You can also schedule an appointment online through our website. Experience the convenience, comfort, and expertise at London Private Ultrasound.
We look forward to assisting you with your healthcare needs and ensuring you receive the best possible diagnostic care.
EXCELLENTTrustindex verifies that the original source of the review is Google. Amazing service as usual. Dr Rez is very kind and gave me a lot of valuable information after my ultrasound. He also followed up with a call to ease some of my worries I had about my results. Would definitely recommendPosted onTrustindex verifies that the original source of the review is Google. I needed an Echo before trialling some new medication. London Private Ultrasound were excellent. I was able to make an appointment at short notice (and postpone it because of a sudden back injury) and the price was competitive. I received the report on the same day and it was very detailed. The Cardiologist was lovely and happy to answer my 'lay' questions! I would highly recommend 🙂Posted onTrustindex verifies that the original source of the review is Google. Dr Reza very thorough and experienced. Saw us on time . Easy to book . Comprehensive report arrived immediately. If you have a wheelchair, let them know in advance and they will do everything to accommodate you and put out a rampPosted onTrustindex verifies that the original source of the review is Google. I booked in for a breast ultrasound with Mr Eduardo Murakami at the St.Albans clinic. An absolutely fantastic service from start to finish and extremely professional. Everything was explained in detail and the procedure was painless and not hurried at all. I received my results via email the same day. All in all, a great experience and I would highly recommend them. The staff are incredibly friendly and polite. Many thanks again, keep up the great work.Posted onTrustindex verifies that the original source of the review is Google. FantasticPosted onTrustindex verifies that the original source of the review is Google. Highly recommended. A very professional and caring team. I was seen promptly over the bank holiday weekend for severe pain, and received excellent service from Dr. Salehi Very happy 😊Posted onTrustindex verifies that the original source of the review is Google. Got an appointment really quickly, service was good and I received the written email report before I got home .
London Private Ultrasound Clinic
At London Private Ultrasound all our services, our specialists and us using the latest Ultrasound technology is designed to deliver the greatest possible experience for all our patients and visitors.
We are conveniently located in Welbeck Street, a stone’s throw from the famous Harley Street and our clinic is a place where you will be welcomed by our friendly staff and feel comfortable in our safe, clean, and reassuring environment.
Address: 27 Welbeck Street, London, W1G 8EN
Tel: 020 7101 3377

